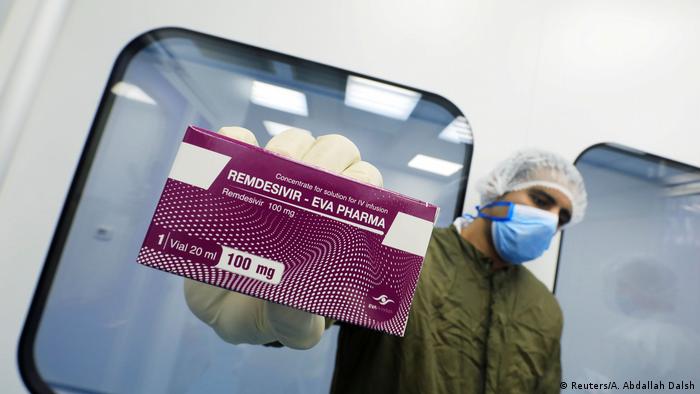
Zolgensma, a gene therapy medicine for treating spinal muscular
atrophy in children under the age of two, is now available in Germany.
However, a single treatment of the drug, which is produced by Swiss
pharmaceuticals company Novartis, comes at the steep price of €1.9
million ($2.1 million).
The manufacturer argues that this is a
reasonable price considering that without it, it costs between €2.5 and 4
million to treat the degenerative disease over a lifetime.
Gilead Sciences, which has developed remdesivir, takes a similar line of argument, saying that the drug, which is
viewed as a promising tool in the fight against COVID-19, could save costs in the long run.
In
an open letter earlier this week, Daniel O'Day, chairman and CEO of
Gilead Sciences, wrote: "Taking the example of the United States,
earlier hospital discharge would result in hospital savings of
approximately $12,000 per patient. Even just considering these immediate
savings to the healthcare system alone, we can see the potential value
that remdesivir provides."
"We have decided to price remdesivir
well below this value," he continued. "To ensure broad and equitable
access at a time of urgent global need, we have set a price for
governments of developed countries of $390 per vial. Based on current
treatment patterns, the vast majority of patients are expected to
receive a 5-day treatment course using 6 vials of remdesivir, which
equates to $2,340 per patient."
Read more:
Remdesivir is no miracle cure

A single treatment of Zolgensma, produced by Swiss pharmaceuticals firm Novartis, costs €1.9 million
What is fair drug pricing?
The editor of the German specialist magazine
Arznei-Telegramm,
Wolfgang Becker-Brüser, is not convinced. He told DW that the costs of
treating COVID-19 without remdesivir had been calculated at random.
"There
is an attempt to give the impression that the price is fair," he said.
"However, if there wasn't a pandemic and so much public attention they
might have set the price much higher."
The Association of
Research-Based Pharmaceutical Companies (vfa) refused to comment. "The
vfa does not comment on the pricing schemes of individual companies," it
said in a statement to DW.
But in the past, the vfa has called
on the pharmaceuticals sector to show responsibility with regard to
consumers and demanded that affordable medicine and vaccines be made
available.
An analysis by British researchers cited in the Germany weekly
Der Spiegel came to the conclusion that it probably cost about €8 to produce one dose of remdesivir.
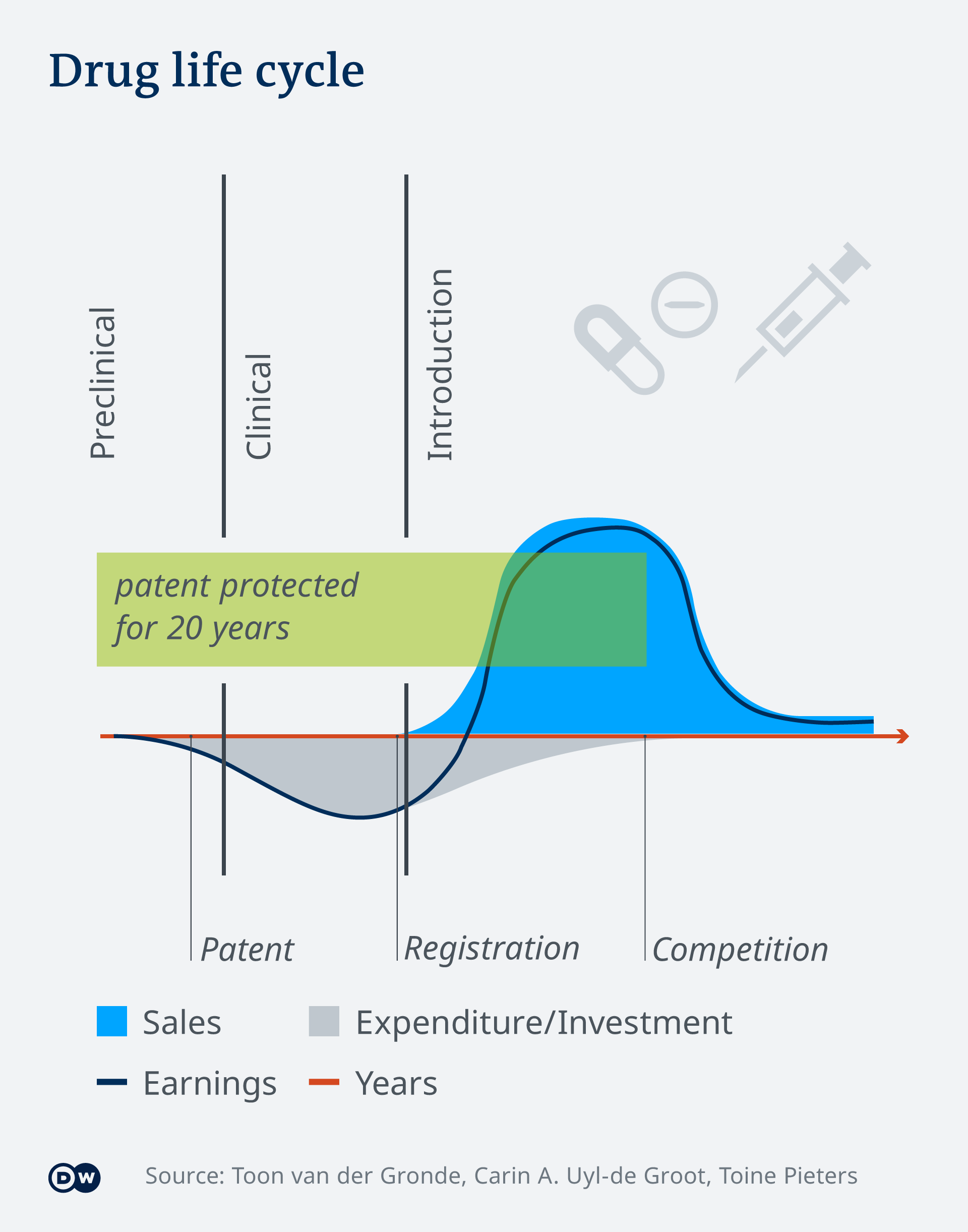
However,
it is normal for the sale price to be much higher than the production
price, considering companies invest huge sums into development.
Read more:
How lab animals have fared in the coronavirus crisis
Gilead
Sciences claims that it invested about $1 billion into remdesivir. This
is actually at the lower end of the vfa's scale for developing a new
drug. The association told DW that companies tended to invest $1 to 1.6
billion in a new product.
For Wolfgang Becker-Brüser, this is "fantasy."
"If the development costs are calculated to be so high then it is easy to demand higher prices," he told DW.
For
Alexander Nuyken, a pharmaceuticals expert at the consulting firm EY,
there is a reason that development costs are so high: they encompass the
risk of failure. "It has to be possible to add a premium for the risks
incurred from the development of a drug to its approval," he said.